Any level of suffering is obviously a concern for everyone, but tackling severe suffering should be a top priority.
Dr Penny Hawkins, RSPCA
What is ‘Severe’ Suffering?
Within the UK and the European Union, ‘severe’ procedures are those where animals used in science are likely to experience:
- severe pain, suffering or distress
- long-lasting moderate pain, suffering or distress, or
- severe impairment to their wellbeing or general condition
%
of animals used in experiments worldwide experience ‘severe’ suffering
animals across the world experience severe suffering each year
procedures involving severe suffering each year within UK and EU
Progress So Far
67%
Reduction
IN EXPERIMENTAL PROCEDURES CAUSING SEVERE SUFFERING IN THE UK Since 2014
The Content of this website is relevant for:
THE ROADMAP TO REDUCING SEVERE SUFFERING
Culture
Analysis
Evaluation
Identify
Issues
Issues
Overcome
Obstacles
Obstacles
Practical aspect
Reports
Avoiding mortality
Experimental Autoimmune Encephalomyelitis (EAE)

Rheumatoid arthritis
Seizures, convulsions and epilepsy
Sepsis
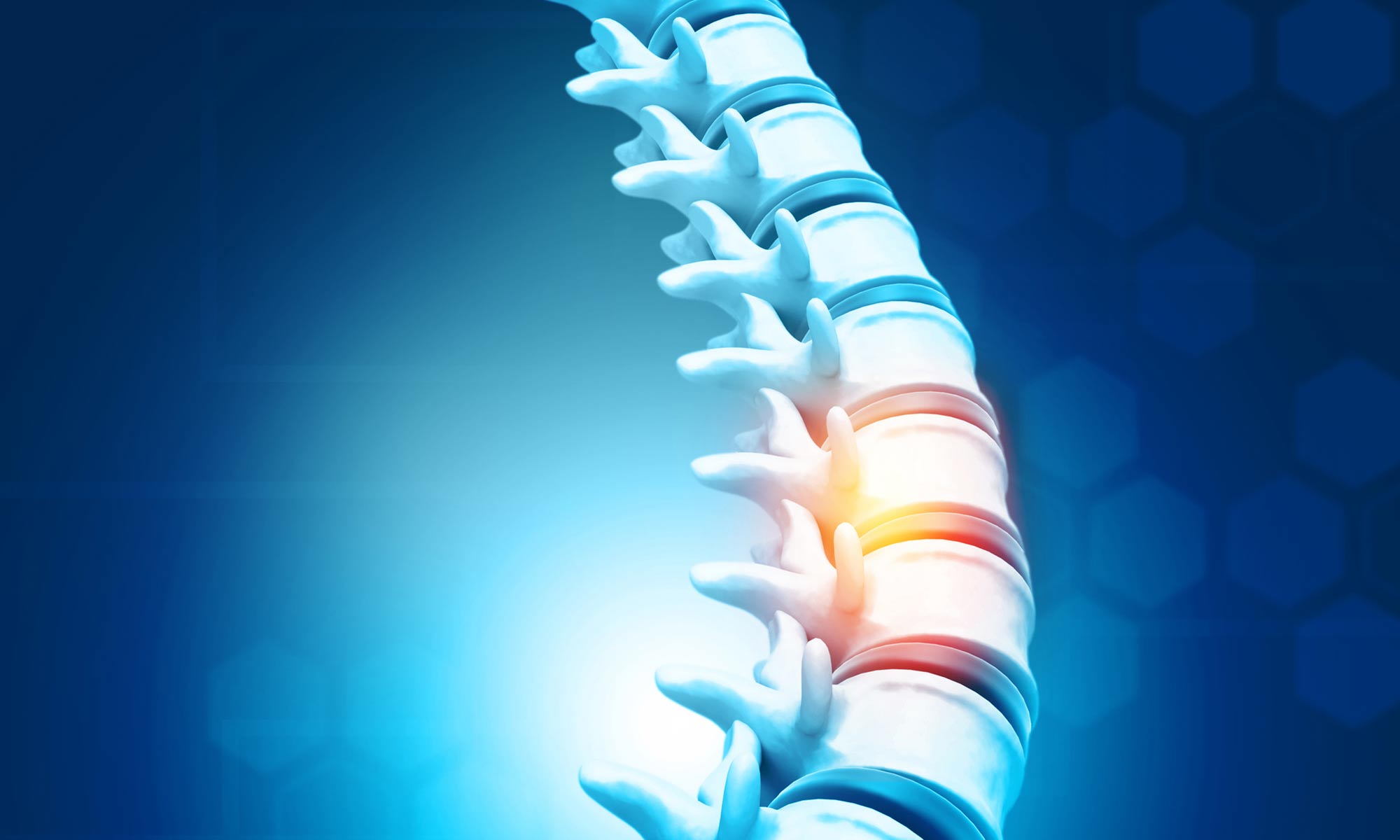
Spinal cord injury

Cardiovascular research

Neuropathic pain

Events
RSPCA has held a series of events, bringing together hundreds of people from across the world, to share knowledge and ideas, and promote practical approaches to avoiding and reducing severe suffering
Read more
Latest
Caring staff are key to reducing lab animal suffering, but the emotional toll can be heavy.
Read more
Ethics
Procedures that can cause severe suffering are of particular concern and the justification for using these deserves special scrutiny.
Read more